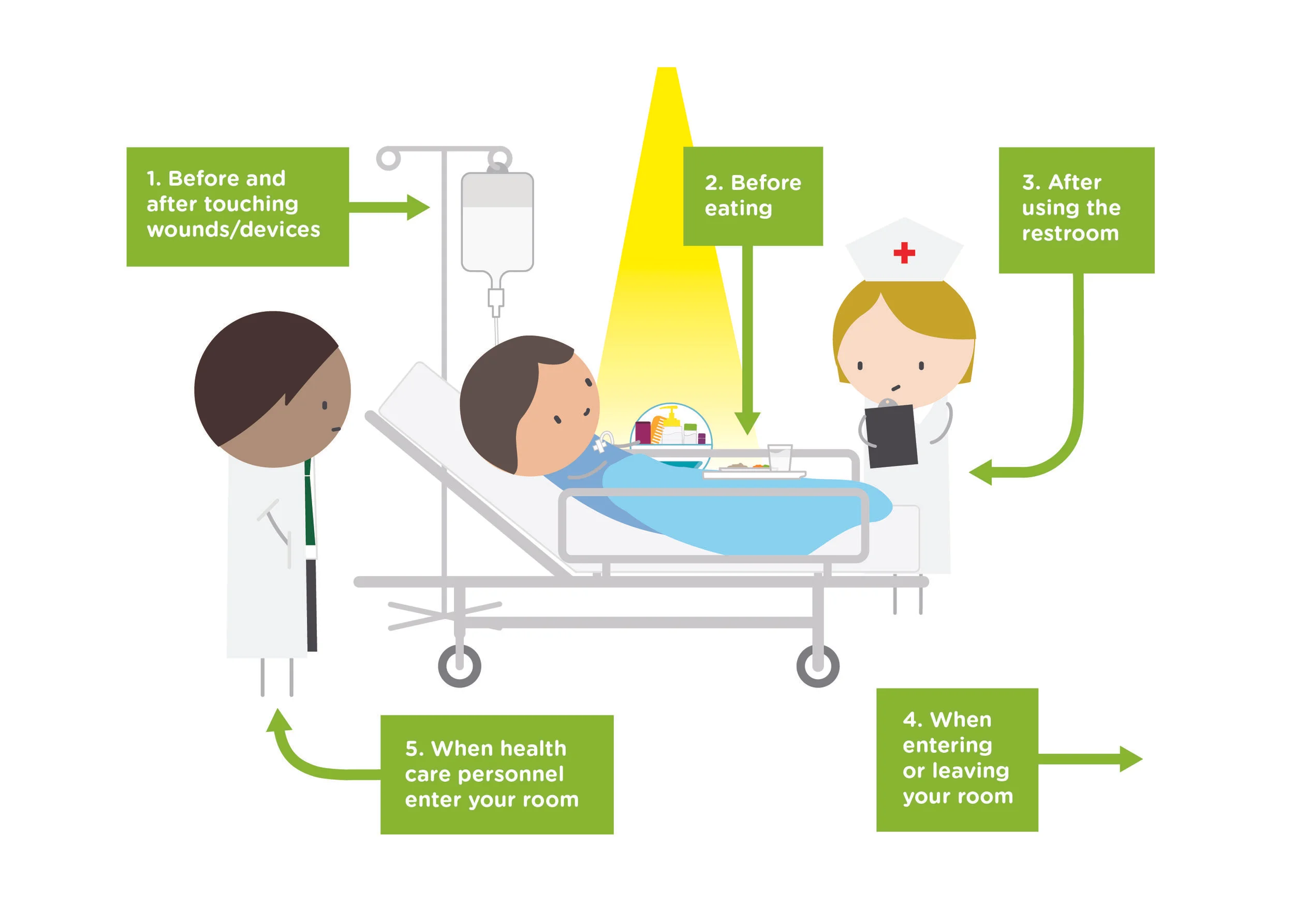
Providing hand hygiene supplies along with educating patients and visitors about the importance of hand hygiene is critical.
A Nurse’s Perspective
A letter from Fitsi Health founder, Kathleen Puri, MSN, RN in The New York Times:
Fitsi Health Founder Wins American Nurses Association Innovation Award
The Infection Prevention Strategy Honors Fitsi as One of the Top Innovations of 2018
Empowering Patients is Critical to Decreasing HAIs
Hand hygiene is the best method to prevent the transmission of infections. Hand hygiene for hospitalized patients sounds obvious – something that should be easy to accomplish and regarded as important to the patient experience. However, patient hand hygiene is a problem for most hospitals today. It is difficult to accomplish and not monitored by healthcare personnel. No infection preventionist will argue against the importance of patient hand hygiene. However, since it is neither prioritized nor measured by hospitals, it falls through the cracks. This, coupled with the fact that more and more research points to patients as the “missing link” in infection control efforts means that, in order to reduce hospital acquired infections (HAIs), hospitals need dedicated efforts to improve patient hand hygiene. Key to achieving these efforts is empowering patients to make hand hygiene easy to do on their own and to understand the critical importance cleaning their hands plays in preventative care.
This Patient-Centric Tool Tackles the Massive Challenge of Hospital-Acquired Infections
Kathleen Puri had been a nurse for many years, but it wasn’t until she became a hospital patient that the issue of hospital patient hygiene began to truly bother her. She noticed that patients confined to a hospital bed had no way to conveniently and easily wash their hands — one of the easiest ways to prevent the almost 100,000 deaths (more than those caused by diabetes or breast and prostate cancer combined) attributed to infections acquired in hospitals annually.
A Win-Win for Hand Hygiene
Holiday Babies and Their Moms Love Fitsi
New moms love Fitsi! Check out this heartwarming video of holiday newborns at St Joseph hospital.... you can see Fitsi hard at work to keep mom and baby infection free!
FDA Warns Against Triclosan
The Federal Drug Administration (FDA) recently stated soap and water are preferable to antibacterial liquid products for everyday use. This is an important issue for consumers. One of the problems with liquid antibacterial soaps is that many contain triclosan and animal studies have shown that triclosan may affect how our hormones work and impact antibiotic resistance.
The safety of products with triclosan is in question. Triclosan is in a large variety of products, many of which are used in healthcare.
When Fitsi Health was making manufacturing decisions the goal was to make Fitsi® as durable as possible. The decision was made to include an antibacterial agent into the plastic we used to make the injection molded bedside caddy. Some people recommended triclosan since it is already used in a variety of healthcare products. But, just as the FDA stated, studies found that hormones and antibiotic resistance may be influenced by triclosan.
As a result, Fitsi Health decided not to use triclosan when making Fitsi® even though it would have been our cheapest option. Instead, Fitsi is imbedded with MicroBlok S. MicroBlok S is a silver ion with a high antimicrobial efficiency that protects Fitsi from staining and deterioration.
Making a product has many dimensions and decisions. Fitsi Health is happy to have made the decision to use MicroBlok S and not use triclosan. Safety is always first!
- Kathy Puri, MSN, RN
Fitsi Featured in Plastics Today
Fitsi bedside caddy promotes patient hygiene
Device integrates antimicrobial technology from Plastics Color Corp.
By Norbert Sparrow
April 29, 2016
A bedside caddy developed by a nurse could help combat hospital-acquired infections (HAIs) simply by making it more convenient for patients to wash their hands. Plastics Color Corp. (PCC; Calumet City, IL), a supplier of custom polymer solutions, compounds, colorants and additive masterbatches with a global footprint, brought its expertise to the project and shared this story.
We are often told that washing our hands is the first line of defense against spreading germs and contracting a cold or the flu. You would think that diligent hand washing would be second nature in a hospital setting, but the facts tell us otherwise. Public health organizations estimate that 1.7 million HAIs occur in U.S. hospitals each year, resulting in 99,000 deaths and an estimated $20 billion in healthcare costs. While basic hygiene is only one of many contributing factors to HAIs, it is a simple and remarkably effective tool. While medical personnel, we assume, follow protocol, several studies indicate that patients do not, as a rule, wash their hands as often as they should. It’s not always their fault. Many patients are bedridden, for example, and it may be painful, even impossible, for them to get to the sink. That is what prompted nurse Kathleen Puri to invent the Fitsi bedside caddy.
The Fitsi bedside caddy allows patients to keep hand sanitizer, lip balm, lotion and other basic care essentials within arm’s reach. It serves as a physical reminder to practice hand hygiene. Designed with a flat bottom and a rotatable clip, Fitsi can sit on a bedside table or conveniently attach to a patient’s bedside rail. A built-in handle allows patients to pick up the caddy and take it to the bathroom.
The Fitsi’s good influence extends beyond the patient. In its press release, PCC notes that hospital visitors are derelict when it comes to washing their hands, and, citing a New York Timesarticle, that even “hospital workers wash their hands as little as 30% of the time that they interact with patients." In this context, the Fitsi serves as a physical reminder that will help patients, their caregivers and their visitors to practice good hand hygiene, notes PCC.
Considering that the device is designed to help patients avoid infections, it’s only fitting that the Fitsi have built-in antimicrobial features, says PCC. Puri and her team settled on MicroBlok S, an antimicrobial formulation developed by PCC.
MicroBlok S inhibits the growth of a broad spectrum of microorganisms on surfaces, reduces stains and odors, and impedes deterioration thanks to the uniform dispersion of silver ions throughout a polymer matrix. The silver ions create a large internal-specific surface within the polymer, producing high-efficiency antimicrobial action, according to the company. The antimicrobial effect is not diminished over time, and the MicroBlok product line can be custom blended in a variety of resins, including TPU, PC, ABS, PP, and PE.
Chattanooga Business Radio Interview: Fitsi Health Founder Kathleen Puri
Listen here to Chattanooga Business Radio's interview with Fitsi Co-Founder Kathleen Puri. Kathy was given the opportunity to share the story of Fitsi Health and how the company is helping to achieve the goal of zero preventable hospital deaths by 2020. Kathy talks about how Fitsi is much more then a bedside caddy - it is part of the Patient Safety Movement and how important it is to advocate to improve patient safety.